Five Tests to Tell If You Have Hashimoto’s Disease
| | Reading Time: 6 minutes

Lab testing is a cornerstone of clinical diagnosis. Because Hashimoto’s disease is the most common cause of hypothyroidism, accurate testing is key to knowing if an underperforming thyroid gland causes chronic fatigue.
Hashimoto’s disease is the most common autoimmune thyroid disorder. No one knows why this happens, but for various reasons, the immune system sets out to attack the thyroid gland. Over time, the thyroid gland is destroyed by your body’s lymphocytes, a type of immune blood cell. Lymphocytes produce inflammatory cytokines like Interleukin 17 that drive autoimmune activity in the thyroid gland. A tipping point occurs when thyroid cells can no longer produce enough hormones.
Well before that stage, however, your pituitary gland responds by making more thyroid-stimulating hormone (TSH). At the same time, your thyroid hormones become deficient. The pituitary is the “master” gland regulating hormone production in the body, including secreting TSH.
When main thyroid hormone levels of thyroxine (T4) and triiodothyronine (T3) decline, your anterior pituitary responds by secreting TSH to stimulate thyroid cells to produce more T4 and T3. You can check your TSH level with a simple blood test.
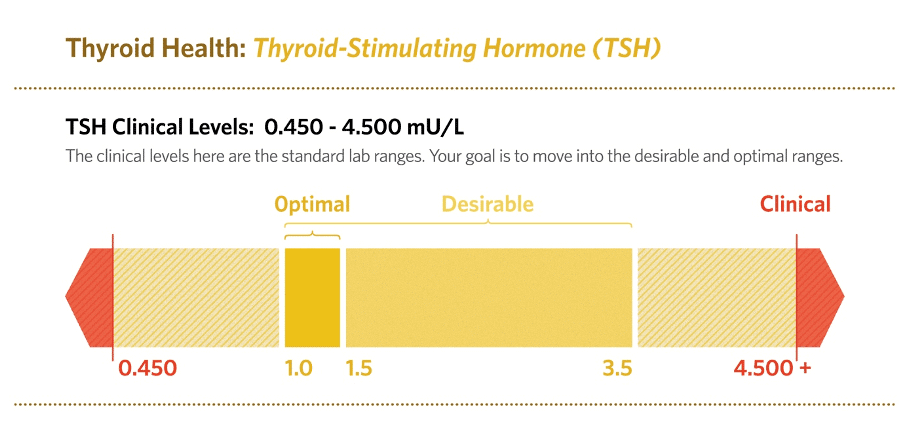
When TSH goes over 4.500 on a blood test, it means that the pituitary signaled your thyroid gland to produce more thyroid hormones. A high TSH is the hallmark of hypothyroidism. But damaged thyroid tissue caused by autoimmune activity associated with chronic inflammation cannot produce enough hormones. The pituitary responds and TSH rises. Some Hashimoto’s patients have TSH levels over 100!
But long before the advanced stages of Hashimoto’s disease, you may have no symptoms at all. It’s at this stage that many get misdiagnosed as depression or not enough sleep. Alternative practitioners blame it on stress-induced adrenal burnout. However, Hashimoto’s patients often have high cortisol levels, not low levels in a blood test. Both views are inaccurate. Hashimoto’s is an autoimmune disorder more complex than simple hypothyroidism that doesn’t lend to simplistic explanations.
Though it’s physiologically accurate that fatigue and depression, and adrenal gland imbalances often accompany Hashimoto’s, only precise diagnosis leads to effective treatment. That’s why it’s crucial to test for Hashimoto’s early in the diagnosis of hypothyroidism.
Common Symptoms of Hashimoto’s disease:
- Unrelenting fatigue
- Weakness
- Pale, puffy face
- Anxiety and panic attacks
- Depression
- Dry skin
- Water retention
- Forgetfulness
- Trouble finding words
- Sensitivity to cold
- Hair loss
- Heavy menstruation
- Unexplained weight gain
- Constipation
As your thyroid gland weakens, symptoms gradually appear. At first, you may feel tired without reason. You might even wake up tired. Your skin and hair become dryer. You feel cold, even in warm weather. You have less appetite but gain weight.
Over time, other symptoms occur, including: poor digestion, constipation, and carotenemia, a yellowish-orange color of the palms.
Hashimoto’s disease was named in 1957 after the Japanese physician Hakaru Hashimoto of Kyushu University. It was the first identified organ-specific autoimmune disorder.
What’s the Difference Between Hashimoto’s disease and Hypothyroidism?
If you complain to your doctor about fatigue lasting months, you’ll likely get screening tests for infections, anemia, and hypothyroidism. You may get labeled as having chronic fatigue syndrome (CFS).
The standard thyroid profile includes free thyroxine index, T3 uptake, thyroid-stimulating hormone, and thyroxine (T4). But most conventional doctors only test TSH. If your TSH is high, your medical doctor will diagnose hypothyroidism and prescribe synthetic thyroid hormone replacement therapy. Synthroid or generic levothyroxine is the most common thyroid hormone prescribed in conventional medicine.
If you see a naturopathic doctor (ND) or a medical or osteopathic doctor practicing functional medicine, you’ll most likely get a prescription for desiccated thyroid hormone. The most common desiccated thyroid medications are Armour Thyroid and Nature-Throid containing both T4 and T3. Desiccated thyroid hormones are made from animal thyroid glands, so they are unacceptable to vegans.
Because desiccated thyroid medication is a complete form of thyroid hormone replacement, in addition to T4 and T3 it also contains thyroglobulin (TG), a binding protein that helps carry T3 in the blood. TG may trigger an increased autoimmune reaction making your symptoms worse. However, most Hashimoto’s patients improve with desiccated thyroid replacement and prefer it over synthetic T4 and T3.
If your doctor takes an integrative approach, your therapeutic plan may include supplements like vitamin D3, vitamin A, selenium, and the amino acid L-tyrosine to support thyroid function. Sometimes, practitioners prescribe iodine if your level is low on a blood test. But, many functional medicine doctors consider iodine contraindicated in Hashimoto’s because it can overstimulate thyroid peroxidase antibody (TPO Ab) if taken in excess. So before you supplement with iodine, test levels in your blood to make sure you have enough but not too much.
If you have Hashimoto’s, be cautious about taking too much iodine. Read the labels on your other supplement bottles, especially multivitamin and mineral and tyrosine products because both likely contain iodine.
Even though autoimmune thyroid conditions are more common than a few decades ago, it’s surprising that conventional doctors still do not routinely screen patients for Hashimoto’s.
The Gender and Gene Connection
Women are three times more likely than men to develop Hashimoto’s. Some studies show that Hashimoto’s is 5 to 10 times more common in women than men. And other gender-specific associations cluster with Hashimoto’s. For example, researchers found that increased breast density occurs more often in women with Hashimoto’s.
Hashimoto’s tends to run in families. At least three genetic mutations can trigger thyroid autoimmunity. Scientists are confident that the HLA family of genes plays a significant part in the autoimmune cascade that leads to Hashimoto’s. However, there is no readily available test for these genetic markers.
Another reason early identification matters is Hashimoto’s autoimmune thyroiditis is often a pivotal dysfunction in other autoimmune diseases. For example, lupus and autoimmune gastritis occur in up to 40% of Hashimoto’s cases.
Do you Have Hashimoto’s disease? How to test for Hashimoto’s?
The first step in diagnosing Hashimoto’s is assessing symptoms. However, the list of symptoms is long and overlaps with other conditions. That’s one reason why Hashimoto’s gets misdiagnosed as chronic fatigue syndrome, adrenal fatigue, depression, or fibromyalgia.
The second step is an examination. Your doctor is well-trained to assess the size of your thyroid. An enlarged thyroid gland is called a goiter. But even a slightly enlarged thyroid signals trouble.
Distinguishing hypothyroidism from Hashimoto’s by symptoms alone is not easy because both conditions share similar indications. However, one of the hallmarks of Hashimoto’s is swollen lymph nodes under the chin in the front of both sides of the neck. You can feel these for yourself.
There is not a single on-time hashimoto’s disease test. A profile of blood tests and an ultrasound scan of your thyroid gland is the only sure way to know if you have Hashimoto’s.
5 Tests for Hashimoto’s disease:
- Thyroid-stimulating hormone (TSH)
- Free liothyronine (T3)
- Free thyroxine (T4)
- Thyroid peroxidase antibodies (TPOAb)
- Thyroglobulin antibodies (TGAb)
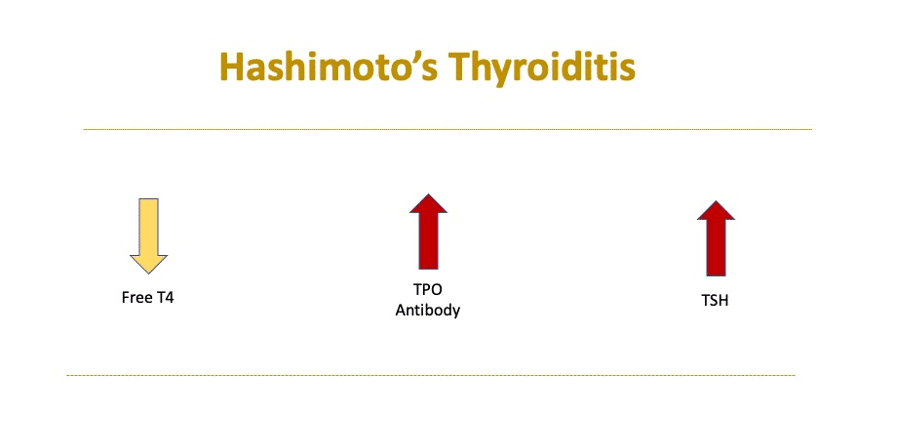
You very likely have Hashimoto’s disease if your TSH is high, your free T4 is low, and your TPO Ab is elevated. High TPO Ab is the key marker because it is present in over 90% of those with Hashimoto’s. TG Ab is present in about 80% of cases.
Getting Your Blood Drawn
Thyroid tests require a blood sample. If you order your blood tests online, or if your doctor writes a requisition for thyroid hormone testing, you have to schedule an appointment at a laboratory’s draw center, like with Quest Diagnostics or LabCorp, or at an independent draw center like AnyLabTest. You can also have a mobile phlebotomist take your blood sample in the privacy of your home. A nurse or phlebotomist will access one of your veins, usually just below the elbow, withdraw enough blood into one or more glass tubes, and process the sample for shipment to the laboratory for testing. On average, your results will be ready in less than one week.
Get your TSH and other thyroid tests done in the morning. Afternoon values tend to be lower. Don’t take supplements or other medications the morning of your blood draw because they can interfere with the test results. A fasting test is best, so skip breakfast. And don’t take your thyroid hormones until after your blood draw.
Hashimoto’s Disease FAQs
Is there a root cause for Hashimoto’s?
Does Hashimoto’s originate in the gut?
How do I know for sure if I have Hashimoto’s?
How to test for Hashimoto’s
Is there a Hashimoto’s disease blood test?
Summary
Hashimoto’s disease is more common than previously thought. Despite the high incidence of Hashimoto’s, this debilitating condition remains poorly understood and often is underdiagnosed and goes undertreated.
If you are female, already have hypothyroidism, or have Hashimoto’s disease in your family, get screening tests for Hashimoto’s. Your doctor, nurse practitioner, or physician’s assistant can order thyroid tests.
You can also order your tests from independent lab testing services like Ulta Lab Tests or membership services like Life Extension. These services use the same national labs including LabCorp and Quest Diagnostics that doctors use.
Remember, your health insurance will not pay for self-ordered blood tests. So, shop around for the best price.
References
Cellini, M., Santaguida, M. G., Virili, C., Capriello, S., Brusca, N., Gargano, L., & Centanni, M. (2017). Hashimoto’s Thyroiditis and Autoimmune Gastritis. Frontiers in Endocrinology, 8, 92. http://doi.org/10.3389/fendo.2017.00092
Davies, T. F., Latif, R., & Yin, X. (2012). New genetic insights from autoimmune thyroid disease. Journal of Thyroid Research, 2012. http://doi.org/10.1155/2012/623852
Pedraza-Flechas, A. M., Lope, V., Vidal, C., Sánchez-Contador, C., Santamariña, C., Pedraz-Pingarrón, C., … DDM/Var-DDM-Spain. (2017). Thyroid disorders and mammographic density in Spanish women: Var-DDM study. The Breast, 34, 12–17. http://doi.org/10.1016/j.breast.2017.04.011
Resende de Paiva, C., Grønhøj, C., Feldt-Rasmussen, U., & von Buchwald, C. (2017). Association between Hashimoto’s Thyroiditis and Thyroid Cancer in 64,628 Patients. Frontiers in Oncology, 7(April), 53. http://doi.org/10.3389/fonc.2017.00053
Staii, A., Mirocha, S., Todorova-Koteva, K., Glinberg, S., & Jaume, J. C. (2010). Hashimoto thyroiditis is more frequent than expected when diagnosed by cytology which uncovers a pre-clinical state. Thyroid Research, 3(1), 11. http://doi.org/10.1186/1756-6614-3-11
Stock, G. (2002). Redesigning Humans: Our Inevitable Genetic Future (Houghton M). Boston & New York.
Wang, J., Zhang, J., Xu, L., Shi, Y., Wu, X., & Guo, Q. (2013). Cognitive Impairments in Hashimoto’s Encephalopathy: A Case-Control Study. PLoS ONE, 8(2). http://doi.org/10.1371/journal.pone.0055758
Zaletel, K., & Gaberr, S. (2011). Hashimoto’s Thyroiditis: From Genes to the Disease. Current Genomics, 12, 576–588. Retrieved from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3271310/pdf/CG-12-576.pdf


